In this article, Cliodhna Grady and Natasha Coen, Clinical Risk Advisers, examine why service user identification errors can occur and how health and social care professionals can avoid them.
While conducting analysis of incidents recorded on NIMS, the State Claims Agency's Clinical Risk Unit has noted a number of incidents relating to service user identification. Incorrect service user identification can result in medication errors, transfusion errors, diagnostic errors and procedures being carried out on the wrong person or wrong site. For example, in one incident reported on NIMS, the incorrect date of birth was present on all documentation and ID wristbands. This meant cross-matched blood for the patient could not be used because of the incorrect documentation. It is the primary responsibility of every health and social care professional to check the identity of service users and match the correct person with the correct care, before care is administered.
Risk factors
A number of factors which may increase the risk of service user identification errors have been identified:
- Two service users with similar names or illnesses
- In an outpatient setting, where ID wrist bands may not be used as an information source
- A service user who is non-communicative, unresponsive or confused
- Two records existing for the same service user, e.g. two records with different order of a double-barrel surname
- Inadequate procedures and policies for the correct identification of service users
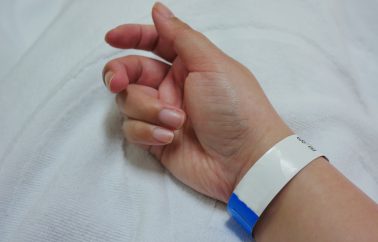

What can you do to minimise the risk?
A standardised approach to service user identification practices across the organisation will help to reduce the frequency of these incidents. Consideration should be given to implementing the following measures to reduce the risk of error:1,2
- ID wristbands should include these four core identifiers: last name, first name, date of birth, hospital / MRN number
- On admission, use at least two identifiers to verify a service user’s identity
- At each encounter ensure the details are correct and up to date
- Ask the service user to identify themselves before receiving any medication and prior to any diagnostic or therapeutic intervention
- Even if the service user is familiar to the health and social care professional, check their details to ensure the right person receives the right care
- Ensure wristbands are legible and replace those that are difficult to read
- Encourage the service user to play an active role in the identification process - empower the service user to speak up when they identify an error relating to their identification, procedure or care plan
- Where service users cannot communicate, e.g. intraoperatively, in the ICU, alternative patient identification methods should be employed
References available on request.
Clinical Risk Insights
Check out more articles from the latest edition of Clinical Risk Insights by the State Claims Agency.







